This is the first of about 6 posts on Social Care that are part of the Politics of Care forum. For more on Teresa Pocock who plays a central role in the efforts of a few of us to define what care is about – see Teresa Pocock.
The Technological Revolution
The technological revolution that took place around 1800 brought with it an awareness of the need for standardisation. This need is inherent in technologies rather than in markets or private enterprise per se. It is critical to efficiency and ultimately trumps, subsumes, swallows both private and public enterprise.
When the first railways were laid in the 1820s, it quickly became clear they had to have the same gauge in different parts of a country and internationally or transport between places would be at least temporarily interrupted. This was more than an irritation when the transport of troops in a time of war was involved.
The nuts, bolts, and screws, and the tools that would manipulate these nuts and bolts, all equally need standardising, as did the later machine tools that led to automation, which by definition, if it works, is completely standardised.
Without standardisation the chemicals, and recipes for mixing chemicals, central to the development of chemical and pharmaceutical industries, wouldn’t work any more than computers can work without standard languages. Chemical reactions require adherence to a recipe, in the way algorithms require adherence to a logic.
Standardisation is an element of logic – it’s a defining of terms. Once defined the terms apply globally, regardless of local factors. This global application supports ‘scaling up’ and quickly became a feature critical to investment by both private investors and public investment in the military, research, and infrastructure.
Once the gadgets and goods that would be consumer goods came onstream, especially those that would be electrically powered, the same logic applied, and common measurements further facilitated both trade and development.
The best options were not always adopted. In early video-recorder days, Betamax was competing with VHS. Betamax was technically superior, but VHS was installed as the standard consigning Betamax to the dustbin of history.
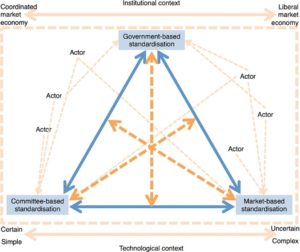
Operationalism
Standardisation is critical to mechanization and a broader operationalism. The advent of mechanization put paid to an artisanat and substituted an unskilled proletariat in their place.
Computerization brought operationalism into view – the broad technique underpinning all technologies. Operationalism can also be taken and applied to organizations and to people and some claim you cannot be scientific without being operational.
Operationalism facilitated further mechanization, increasing the opportunities to shed the skilled workers previously needed to operate many machines. Shedding workers was seen as politically desirable in many industries, even a matter of national security, as the ability of workers in key industries to strike could compromise defence and government.
After 1945, with the advent of computerization, there was a steady fall in employment in manufacturing industry from 80% of workers to less than 10% now. Iconic industries like American Steel and British Coal shut down and with their closure union power collapsed.
This gave rise to a political need to find work for newly unemployed multitudes. A profusion of new goods and machines supported the development of service industries, which had the capacity to absorb large numbers of staff. The service industries had to absorb not just those laid off from manufacturing but also their partners (usually wives) as the collapse of union power meant a collapse in wages making it necessary to have two wage-earners to support a family.
Management
The Second World War and its aftermath also saw a replacement of entrepreneurs by managers. Just as military engagements had, the operations of factories, often huge corporations, essential to defence and government, needed standard operations – processes, and oversight of the implementation of these processes by managers.
In manufacturing industries, this gave rise to tensions pitting managers ‘against’ well-paid skilled workers. The managers might know the on-paper processes better, but the workers knew the idiosyncrasies of machines, even though these were increasingly standardised, and how to make the interface between workers and machines work best.
The managers won out. Skilled staff and bottom-up inputs (entrepreneurial) to development vanished. The business of America was no longer business in the sense of risk-taking – opening up opportunities in a market and moving nimbly in the way that it had been. It was now about risk-management.
The new entities were focussed on a refinement of processes that allowed for outsourcing and disarticulating the enterprise into components. See The Neoliberal Deep State (in 2 weeks time).
The Service Sector
From 1950 through to 1980, the service sector from fast food to retail, hospitality, banking and other services lent itself even more readily to these operational processes than manufacturing had done. Standardization made staff interchangeable and allowed brands like McDonalds and Pizza Hut to scale up and globalize.
With Pizza Hut and McDonalds, the focus was on delivering standard products to people. Quality in these new services changed meaning from delivering the best possible hamburger or pizza to delivering the same product every time. In terms of interactions with the people receiving these products, this could also be standardised into a few ‘Have a Nice Day’ soundbites, with metrics introduced to get feedback on how often staff smiled and how smooth the service had been.
Around 1980, the service industry began to extend to education and both health and social care. Managers were brought in to run these ‘services’, touted as bringing private enterprise into a formerly public sector, or the new public service management as it was termed.
In these cases, however, the services are not simply a matter of delivering standard products to people in a standardized way. People themselves rather than pizzas or hamburgers are the object on which these services can act. Operations on bodies can scale but operations on people can’t, at least not in the same way – the outcomes are too variable.
The changes that took place however transformed universities into an educational services sector, healthcare into health services and social care into social services. They have led to a deskilling of university, health and social care staff, and an increasing number of temporary and poorly paid posts. They have produced tensions between faculty and university management, between medical staff and health service management, and almost universal concern about social non-care.
The changes brought a shift from nuanced education to standardised products. A shift from treating serious disorders for which patients sought help whose outcomes even with the best care were often unreliable, to giving patients disorders for which medical services can offer reliable but irrelevant (and potentially life-threatening) interventions. A shift from bad social care to an even grimmer social non-care.
Care Sector
For centuries up to 1980, the long-term care sector for children, the elderly, the vulnerable and the disabled was run by a range of players from religious orders to other benevolent bodies, private owners, and later with public input from Welfare State Aid through local councils.
The Welfare State input started in England in a rudimentary way with a Poor Law around 1600, which after 1945 evolved into Departments of Social Services.
Unlike Britain’s National Health Service, which from 1948 was free at the point of delivery, the post 1945 Social Care sector continued to have a mix of State provision mixed with personal payments and voluntary service inputs.
If health delivers effective treatments for disorders that impair people’s ability to work, it will in principle fully pay for itself. Social care was different in this sense but, as was recognized in the French Revolution, even though born deaf or blind, with technologies like Braille and techniques like sign languages, it was possible for people to contribute to society, live a fuller life, and at least partly defray the expense of supporting them.
This principle was adopted on an even broader basis after the American Civil War with services for veterans, and then with the creation of rehabilitation services, a mixture of health and social care, after World War I. Broadly similar arrangements applied in most countries.
[There are differences between countries that readers will have to give me some leeway on. These differences have been as great as the differences between American and British medicine, one initially private and other public, but both now close to identical. The concern in these posts is about how two so different systems health systems could end up close to identical – the care sector was never as different between countries but shows striking similarities now – one’s that it shares with health.]
In all countries, pressure to organize the different elements of the social service sector into a functioning unit grew for several reasons.
- An inevitable set of residential/long-term care home scandals in most countries called for increased oversight.
- Falling real wages from the mid-1970s meant more people had to work in paying jobs, making it likely that an increasing number of elderly people, children, or vulnerable/disabled people would end up in a residential facility.
- The growth in the numbers of the elderly, both in absolute terms and as a proportion of the population given falling birth rates, added to the sense of a looming crisis.
Societies have always made some accommodation for the indigent. This need was originally met by religious orders and voluntary bodies. In addition, however, by the 1980s the prospect of a larger scale provision of residences for people who needed support with bodily care and disability management was growing and had two novel features.
Public health nursing had emerged in the United States around 1908, and social work as a profession in the 1920s, with slower developments elsewhere. Comparable developments took place in Europe after 1945. There was however no central body with responsibility for or training in the provision of social services. In addition, to some extent many older people could pay something toward their own care, even if only by surrendering the benefits they were otherwise receiving.
To respond to growing concerns about how to support the indigent, the elderly and the disabled, in addition to providing preventive educational and health services, there was a turn to community care in the 1960s. This led to staff paid by social services calling to people’s homes to support basic meal provision, hygiene considerations and some health issues if the visitors were district nurses. This provision aimed at keeping people in their own homes longer, which was viewed as better for them and more economic.
This turn to community care in social services was accompanied by a de-institutionalization of people with learning disabilities to ‘homes’ where they would be supported by staff, as well mental health patients to hostels or other rented accommodation and elderly persons to ‘places in the community’.
In a number of countries, there was a trans-institutionalization of some, particularly mental health and handicapped persons, from hospital warehousing to prison warehousing rather than to the community care, envisaged in the 1963 US Community Mental Health Act.
A growing number of people in community residential facilities led social services to generate standards for these facilities. Between generating standards, employing some visiting staff, and paying some of the benefits like old age pensions that helped defray the costs of accommodation, social services became a focus for the sector and had to find answers.
Reforms put in place in Britain in 1990 endorsed the idea of a purchaser provider split in both health and social care. The purchasers of ‘care’ would put standards in place and would expect to see evidence of these being met.
This made it possible for social service (and health) departments with a brief to fund social care to contract out to groups who claimed they had expertise to do the job. This included private sector operators. In Britain in 1975, there had been 18,800 private sector residential facilities. By 1990, there were 119,900.
The introduction of standards helped lead to a consolidation, which increasingly after 1990 was billed as bringing private sector responsiveness to ‘caring’, an openness to innovation, a culture of quality improvements, investments, and services that would be economically sustainable.
Corporate development of this sort requires managers whose focus is primarily on bureaucracy rather than enterprise. This focus can produce apparent quality improvement as the tick-boxes get checked. If we neglect the aphorism that not everything that counts can be counted, the operation can appear to be functioning well, even improving, and evidently appear to be value for money.
Introducing standardization made staff interchangeable, which supported downward pressure on wages. It also opened up the possibility of a group taking over a number of facilities, financed in part by introducing efficiencies/economies such as standardising meals which allowed for bulk buying with unit costs becoming cheaper the more facilities were part of a corporation.
In Britain, research by Sheffield Hallam University found that around 2017 care homes with mainly council-funded residents were spending less on average on food and drink per patient per day than the cost of a high street coffee.
This corporate development in response to regulation fits a pattern found from food to drug regulation. Regulations/standards promote corporate development and with this comes a greater focus on operations that support scaling up, calling for further corporate growth.
In this case there was an expansion into retirement homes, assisted living facilities, and nursing homes, offering a one stop system for the elderly, the infirm and the disabled (and their families).
The developments included contracting out from the centre. The parent company can contract out the hiring of staff to work with residents to one company and cleaning staff to another company etc. In all cases, this contracting out leads to competition between providers and depresses wages but also inhibits the ability of anyone to notice things that may be going wrong and to push for them to be put right.
On the ground, families concerned about a relative were increasingly faced with managers whose job was to resolve complaints rather than solve problems. Families no longer got to meet someone who could make a meaningful difference in the way that taking an issue to a voluntary body or owner once could.
In Britain, and likely everywhere else, there is evidence that when relatives complain about abuse or neglect, care homes ban visits, or residents are evicted.
The charity Action on Elder Abuse estimates that around 100 elderly residents are abused in care homes every month, including physical and sexual assaults and theft. Very few of these are reported.
In most countries in the years between 2000 and 2020, there was a consolidation of the ‘market’. In Canada four major chains now own a majority of facilities (Revera, Chartwell, ExtendiCare, Sienna Senior Living).
In Britain, 5 companies do – HC-One 21,000 beds, Four Seasons Health Care 17,000 beds, Barchester Health Care 12,500, BUPA 7,700, Care UK 8,000, with many of these companies effectively owned by Hedge Funds, who extract as much profit as possible in order to pay down the debt incurred on purchasing these businesses with guaranteed revenue streams. Four Seasons declared bankruptcy just before Covid creating a real crisis in terms of where their residents and staff might go.
In the US eight companies dominate: Brookdale Senior Living, Genesis Healthcare, Golden Living (owned by GGNSC Holdings), and HCR Manor Care, along with Bupa (UK), ExtendiCare (Canada), Korian and Orpea (France).
By 2020, many of these companies were making tens of millions of dollars profit annually and their share price and director compensation was beholden to these profits. The directors had backgrounds in real estate, hospitality, finance, insurance, pharmaceuticals, or other private health service companies (service sector backgrounds). Virtually no-one on any of these boards knew much about care home coalface issues. See Press Progress.
Covid and Care
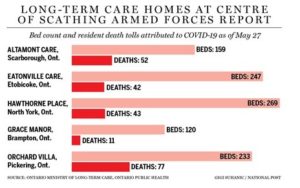
In 2020, the Covid crisis put excess deaths in long term care facilities on the public’s radar, exposing rotting fixtures behind apparently quality facades. See Ryan Tumilty.
Emergency staff (the military in some Canadian cases) put into the facilities found rotting food, insanitary conditions, not enough staff, and arguments between staff that interfered with care. There was a lack of PPE, and staff were so poorly paid that many had to do several jobs, in the process tracking from facility to facility, almost certainly contracting and then spreading the virus.
The response of management to the crises was to offer to:
“implement additional measures, processes and protocols”.
But also noting that:
“Any shortage of qualified personnel and general inflationary pressures may require the company to enhance its pay and benefits package to compete effectively,”
“An increase in labour-related costs or a failure to attract, train and retain qualified and skilled personnel may have a material adverse impact on the business, operating results and financial condition of the company”.

Another more recent response from management and politicians has been to focus on vaccinating care home staff as the answer. This technical solution to a people problem in between the lines blames people whose behaviour has been dictated by poor pay. A solution more appropriate for bodies than for people.
Another longer-term technical solution to Care Home issues mooted has been to introduce robots as companions for older people and others in LTC.
Technical solutions like these mirror Geo-Engineering suggestions as a response to climate change – let’s blot out the sun with reflectors. If believing in technical processes to the point where we allow them to trump judgement calls, as Shipwreck argues, has landed us in the mess we have, then these technical solutions are not the way to go, unless applied within a framework which sees the need to ensure that techniques enhance rather than diminish us.
In terms of Canadian LTC deaths, these have been two-fold greater in for-profit facilities compared with non-profit facilities and four-fold greater than in municipal facilities. The non-profit sector demonstrates that there are other ways to keep costs down than outsourcing staff. If facilities are local, it becomes possible to have family members or others in as volunteers, keeping staff costs down but also having someone able to spot problems and willing to speak up before a problem becomes costly.
NB
On July 21 the Care Quality Commission in England released figures on deaths in Care Homes in England between April 2020 and March 2021 – there were over 39,000 which was close to one third of all deaths in England during this period.
See Worst Affected Care Homes and Nearly 40,000 Care Home Covid Deaths. The CQC give the Breakdown for each Home, while stressing that Deaths are not a good indicator of Care. There are some very bad ‘private’ home figures and equally bad ‘public’ home figures.
A huge factor in this case appears to be have been the Conservative Government with Boris Johnson apparently saying Its only the over 80s who are dying and the Government creating the biggest super-spreader event of all time by dumping thousand of elderly people out of Hospitals and into Residential Facilities where they were being looked after by people so poorly paid they were working in several different facilities. The government now plans on making vaccinations mandatory for Care Home staff.
Social Care Crisis
Before Covid happened, a growing number of people had been drawing attention to the crisis in this sector. The books below outline a crisis as intense as the climate crisis but one receiving less, almost no, attention.
Lynne Segal and Colleagues wrote the Care Manifest0.
Emma Dowling The Care Crisis
Greg Gonsalves and Amy Kapczynski put together The Politics of Care
Madeleine Bunting wrote Labours of Love
These books reflect on a catastrophe unfolding in front of us. Before things became this grim there was Joan Tronto’s Caring Democracy
And perhaps the greatest ever book about Health and Care – Annemarie Mol’s The Logic of Care. The Dutch cover of her book is much better than the English one – once you read the book you realise this cover tells you a lot of what you need to know about Care.
These books tackle the crisis and the meaning of the crisis. Pat Thane has been the person who has done most to put the history of the care sector on the map and the linked need for us to do something rather than just let things drift. She has been a driving force behind many reports on the issues while keeping her name in the background.
See Unmet Need. Social Care Human Rights Watch Report 2019.
What is Care?
This Politics of Care forum was born from a sense there is a connection between what happens in institutional ‘care’, or settings where racism and class bias come into play, and our abilities to help when someone has an adverse effect on a drug.
In all cases there is a growing invisibility, the answer to which is not a wiping of bottoms, but a standing up to something. Wiping bottoms can be slave labour rather than care. And we seem increasingly enslaved.
How do we restore Care? Read Ways you can Save the World and ask yourself if you have the guts to do any of this. If its not scary, and you think it doesn’t take guts, you don’t understand what’s going on?
If you don’t actually do it, do you think you can Care?
If your doctor doesn’t respond by taking your side, do you think s/he can Care?
If the politician you might vote for hasn’t got the guts to call out a ghostwritten literature and lack of access to clinical trial data, is s/he going to perpetuate the system rather than make the kind of difference we need?
(There is at present no politician or party that has stepped up to the plate – not the Labour Party in Britain, or Green parties in Europe, or Sinn Fein who began life as a co-operative movement – we will keep you posted if this changes).
We need to find a way to marry the wonderful analyses of caring cited above, with things that might seem technical and not much to do with care until you realise that there is something badly wrong with techniques like randomized controlled trials and evidence based medicine, when they leave Carers (doctors and nurses) dismissing, even laughing at people who have been made intensely suicidal on antidepressants or had their ability to make love wiped out permanently.
You may know psychologists, social workers and others involved in care, who are happy to ventilate uselessly in the abstract about the problems drugs can cause. You might think they are on the right side, but you won’t know that almost to a person they are scared silly to speak up about the problems they see treatments causing specific people. This may be because they too are trying to understand what is going on and establish where they can really make a difference – but Rome continues to burn while they grapple.
It would be good if anyone reading this can draw the forum and its issues to the attention of as many people as possible – not as an answer to what we should do. but as offering some specific to-dos that might shed some light on what it is we are grappling with – if someone tried them out.

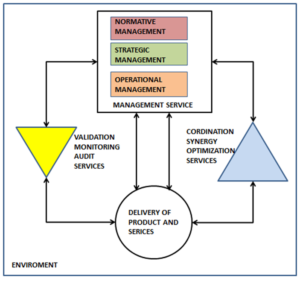











I.ve already written to umpteen ‘care home’ managers flagging up the over medication issue inviting them to contact me initially if they wish so I can forward enquiries and giving DH contact e mail. -with some info carefully edited from the blogs What they want is ‘stories’ to add to their campaigns but it seems others with expertise can be seen as a challenge to their own org. not as collaborators. It includes this group which has done a lot to highlight the issues -but no response. I just flag this up as a dead end attempt which mirrors trying to get a response from other orgs such as Social Services and Elderly People and Childrens Commissioners . From just personal experience The worst thing about reporting a ‘concern’ about the care of friends or something seen in a ‘home’ is fear of repercussions on them. It could be someone knows a better way of getting a response from any of them…
I tried this group several times as they were in the news a lot and seemed to be doing good work -no response
Click here to download the report
CCFTV included in submission to the Law Commission
Care Campaign for the Vulnerable has been included in a submission to the Law Commission on abuse of our elderly to be made ‘hate crimes’. Click the button below to view the submission…
Click here to view the Law Commission submission
The CCFTV Organisation
Care Campaign for the Vulnerable (CCFTV) CCFTV – TOGETHER, WE WILL MAKE A DIFFERENCE (‘Together’? Orgs don’t seem to want to collaborate with others though) They don’t ultimately want to risk it might rock their boat
Care Campaign for the Vulnerable was one of the first organisations to call for a public inquiry way back in April 2020 and so we are now pleased to see a commitment from the Government to hold a public inquiry on the handling of care homes during the Covid 19 pandemic. If you would like to talk to us in confidence about your experience in a care home during the Covid pandemic, please contact us in strict confidence at ccftv.cares@gmail.com
Golden Twilight –
During one of our Canada to Scotland telephone calls, my daughter remarked “thank goodness, Grandma, wasn’t around to go through all this”.
Interesting turn of phrase ‘go through’
Suddenly I had to make real decisions, with far-reaching consequences on behalf of my mother, the brave and fearless women who through her decisive actions had saved me from Seroxat incurring the wrath of doctors along the way – I had no idea my dear, kind, well-mannered mother had it in her to draw on all her instincts to save her remaining offspring…
To keep her self in her lovely home she organised for home-help through an expensive agency. This agency subsequently folded-up despite being one of the leading companies in the field.
Matters came to a head when she had a bad fall. Coincidentally, this was the day I had arranged for an extremely nice senior nurse from a local country-house residential care home to visit her to talk about her future and may be even take her for a visit. When ‘Rose’ arrived, there was an ambulance, a doctor and a carer and mum was on the floor with her glasses on upside-down. Mum was whisked off to hospital and I flew down immediately, Rose having called me.
Two weeks later, mum was a resident.
Mum had quite substantial savings which paid for her new home. After a couple of years, there was no choice but to sell-up her home.
I had no idea that her care home was part of a syndicate of several nursing homes.
The Manageress, tall, slim, attractive, held regular meetings with suited-men who arrived quite regularly for meetings. Not once, in four years, did the Manageress speak to me.
The home seemed relatively faultless. The staff were great, well-organised, there were activities every day and trips to the seaside for fish and chips and ice-creams. Whenever I visited, we loaded the wheelchair in to the hired-car and off we would go, all over Kent.
This post about Care hit a raw nerve with me.
My dear, lovely mum, was over-medicated with morphine, fentanyl patches, gabapentin and doctors talked about other medications. I tried extremely hard to to stop this with doctors who rushed in and rushed out but to no avail, mum died in front of me ‘drug-wrecked’ all the life sucked out of her, a skeletal husk of doctors and their medication-abuse.
What should have been mum’s 100th birthday, on Christmas day 2020, was that what appeared to be a working care system costing a fortune failed her.
Mum had absolutely nothing wrong with her, fit-as-a-fiddle, always well-dressed, lipstick at the ready, we always had a good-time. It had happened again – there was nothing wrong with me when Seroxat was stridently claimed to be effective.
Go-through the Doctor-dominated Matrix or Drive-through the Care-dominated Scheme of Things –
Since Covid ‘care homes’ are no longer such a lucrative business where people have been/are used as commodities and housed sometimes in ‘residences’ as big as warehouses. They are being sold off. ie Peoples’ ‘homes’ are being sold under them and many being told to leave.I would rather see this gross business abolished altogether and taken back into social services if they could sort themselves out and provide a national service of a choice of types of accomodation as individuals desire
S.S had real failings but they neednt be repeated.
carehome.co.uk
Care Homes For Sale in Wales & Nursing Homes For Sale in Wales
Nursing Home – Rhondda Cynon Taff
£475,000 (Freehold)
Rhondda, Cynon, Taff (Care Home / Nursing Home For Sale)
Delightful detached Nursing Home (Registered for 16 residents), peaceful yet accessible desirable setting, South Wales – Fee income £745,319 per annum (y/e 31.03.21) generating an EBITDA of £61,113, operated with experienced
6 hours ago
Redwoods Dowling Kerr
FORMER JUNIOR SCHOOL (CLASS D1 PP) ON SITE AROUND 0.75 ACRES, SUBJECT TO SURVEY
£375,000 (Freehold)
Aberdare, Rhondda, Cynon, Taff (Other For Sale)
Former Junior School on a site of around 0.75 acres/0.30 hectares (subject to survey) in a village location approximately 4 miles from the town of Aberdare and currently with D1 planning permission. Possible
23 May 2021
Bishops
Residential Care Home – Conwy
£995,000 (Freehold)
Conwy (Care Home / Nursing Home For Sale)
Exquisite Detached Residential Care Home for the Elderly (Registered for 16 residents), desirable and accessible location, North Wales – Turnover £469,111 per annum (y/e 30.06.20), impressive EBITDA of £227,737, 14 single & 1 twin
28 Apr 2021
Redwoods Dowling Kerr
Residential Care Home – Denbighshire
Offers Over £2,000,000 (Freehold)
Denbighshire (Care Home / Nursing Home For Sale)
Impressive Detached Residential Care Home (Registered for 32 residents), convenient and accessible location, North Wales – Turnover £901,655 per annum (y/e 31.10.19), impressive EBITDA of £280,545, 30 bedrooms (17 with en-suite
27 Apr 2021
Redwoods Dowling Kerr
Project Liberty – Ref 44531
1600000 (Freehold)
Wales (Care Home / Nursing Home For Sale)
Project Liberty represents the opportunity to acquire a well-established and profitable freehold nursing home in South Wales. The home has enjoyed significant investment over the years and originally two semi-detached properties
15 Apr 2021
Redwoods Dowling Kerr
PURPOSE BUILT NH – Reg 34 (Ref: 4704)
£1,995,000 (Freehold)
Denbighshire (Care Home / Nursing Home For Sale)
DC CARE REFERENCE: 4704 NORTH WALES PURPOSE BUILT NH – REG 34 EXPERIENCED MANAGER IN SITU ASSET SALE GUIDE PRICE £1,995,000
14 Apr 2021
DC Care Specialist Healthcare Business Agents
Group of Nursing Homes – Conwy
Bids Invited (Freehold)
Conwy (Care Home / Nursing Home For Sale)
Group of 2 impressive nursing homes (Reg 44) peaceful yet accessible locations, North Wales. Advised combined fee income £1,803,755 per annum, truly enviable reputations, historically high occupancy, superbly appointed,
03 Dec 2020
Redwoods Dowling Kerr
A HIGHLY REPUTABLE PROVIDER OF DOMICILIARY CARE – REF 161750
Offers Invited (Leasehold)
Wales (Care Provider Business For Sale)
BASED IN WALES Turnover in excess of £925,000. Delivers person-centred domiciliary care services for over 60 clients. Regulated by the Care Inspectorate Wales and is a member of the United Kingdom Home Care Association. Works
18 Nov 2020
Knightsbridge Business Sales
IMMACULATELY PRESENTED CARE HOME – Reg 24 (Ref: 4690) UNDER OFFER
£975,000 (Freehold)
Denbighshire (Care Home / Nursing Home For Sale)
DC Care reference: 4690 – North Wales – UNDER OFFER Residential care home – registered for 24 Consistently good inspection reports Immaculately presented High levels of EBITDA Trades at full occupancy FREEHOLD GUIDE PRICE
02 Oct 2020
DC Care Specialist Healthcare Business Agents
PROFITABLE SPECIALIST CARE HOME – Reg 23 (Ref: 4684)
£1,150,000 (Freehold)
Wales (Care Home / Nursing Home For Sale)
DC Care reference: 4684 North Wales – profitable specialist care home Mental health care home Registered for 23 clients Excellent compliance history Experienced team in place Freehold guide price £1,150,000
28 Sep 2020
DC Care Specialist Healthcare Business Agents
Brigadoon Care Home – Conwy
£585,000 (Freehold)
Llandudno, Conwy (Care Home / Nursing Home For Sale)
Delightful Detached Residential Care Home for the Elderly (Registered for 11 residents), highly sought after & convenient setting, Conwy – Fee income £312,541 per annum (y/e 30.04.20), all room single en-suite, historically high
23 Sep 2020
Redwoods Dowling Kerr
Project Liberty – 44531 – South Wales
1600000 (Freehold)
Swansea (Care Home / Nursing Home For Sale)
Well-established and profitable nursing home registered for 22, providing specialist care for adults with mental health and challenging behaviors. Income of £1,021,465 for the year ended the 31st March 2019, generating an EBITDA
10 Sep 2020
Redwoods Dowling Kerr
Residential Care Home – Cardiff – 47561
£1,400,000 (Freehold)
Cardiff (Care Home / Nursing Home For Sale)
An opportunity to acquire a well-known and highly respected residential care home for the elderly located in a popular South Wales town. Having been in present ownership for over two decades, the home has earned a truly enviable
06 Sep 2020
Redwoods Dowling Kerr
Residential Care Home – Conwy – 47972
£1,100,000 (Freehold)
Conwy (Care Home / Nursing Home For Sale)
Delightful Residential Care Home for the Elderly (Registered for 18 residents), convenient and accessible residential area, truly enviable reputation. “At or approaching 100% occupancy. Rated “GOOD” by CIW. Fee Income £532,357 per
04 Sep 2020
Redwoods Dowling Kerr
Residential Care Home
£550,000 (Leasehold)
Vale of Glamorgan (Care Home / Nursing Home For Sale)
Charming Residential Care Home for the Elderly (Registered for 26 residents), South Wales, excellent reputation, 7 en-suite bedrooms, well presented throughout, Fee Income £897,485 per annum (y/e 31.03.19), impressive EBITDA of
10 Dec 2019
Redwoods Dowling Kerr
Project Stephen – Wales – 45305
£1,000,000 (Freehold)
Wales (Care Home / Nursing Home For Sale)
Project Stephen represents the opportunity to acquire a well established care home located in West Wales. Operating since 1993, the business has developed a fantastic reputation through quality residential care. Ideally located
04 Jun 2019
Redwoods Dowling Kerr
Care Home – North Wales – 46682
Offers Invited (Freehold)
Wales (Care Home / Nursing Home For Sale)
Impressive EMI Nursing & Residential Care Home for the Elderly, registered for 28 residents, peaceful yet accessible setting, Fee income £933,574 per annum (y/e 31.01.20) with EBITDA of £251,460(23%), 26 single&1 twin room (17
04 Jun 2019
Redwoods Dowling Kerr
Domiciliary Care Agency – South Wales – 46832
£175,000 (Leasehold)
Wales (Care Home / Nursing Home For Sale)
Well established & lucrative domiciliary care agency, convenient & accessible trading position, South Wales – Turnover £143,068 y/e 31/10/2017 adjusted net profit of £44,541 (31%) truly enviable reputation, approximately 305 hours
16 Apr 2019
Redwoods Dowling Kerr
Detached Converted Nursing Home
£1,250,000 (Freehold)
Holywell, Flintshire (Care Home / Nursing Home For Sale)
Detached Converted Nursing Home; Registered: 23 service users – category of Older People (N); 17 single bedrooms, 3 twin bedrooms – 7 of which have en-suite facilities; NVQ level 5 Registered Manager with excellent credibility
03 Apr 2019
Cooper Healthcare
Learning Disability Care Home – Wales
£750,000 (Freehold)
Wales (Care Home / Nursing Home For Sale)
Highly renowned residential care home for residents with learning disabilities. Fee income of £310,000+, Registered for 5 residents. Historically healthy occupancy levels. Substantial detached property, Enviable reputation.
22 Nov 2018
Redwoods Dowling Kerr
Care Home – Conwy – 45343
£1395000 (Freehold)
Conwy (Care Home / Nursing Home For Sale)
Highly respected care home for residents with Mental Health (Registered for 23), convenient and accessible setting, Conwy – Fee income £611,366 per annum (y/e 31.01.16), impressive EBITDA, truly enviable reputation, historically
10 Mar 2017
Redwoods Dowling Kerr
CARE HOME – SOUTH WALES – 41136
£450,000 (Freehold)
Swansea (Care Home / Nursing Home For Sale)
Learning Disability Care home registered for 8 residents providing care for Learning Difficulties. Advised fee income (Y/E 29/02/2019) of £244,153 with ANP of £96,201 (39%). End terrace terraced property set in a semi-rural
04 Oct 2013
Redwoods Dowling Kerr
CARE HOME FOR SALE IN POWYS – 41765
£1,900,000 (Freehold)
Powys (Care Home / Nursing Home For Sale)
Impressive detached residential care home, providing care for the elderly and dementia sufferers. Registered for 40 residents. Desirable location.Fee income for Y/E 31/3/2019 £934,247 with an ANP of £254,358 (27%)) 38 single rooms
08 Aug 2013
Redwoods Dowling Kerr
Great more detailed video on All4 (Chanell 4 7pm news today – playback)
Down’s syndrome: Abortion case heads to High Court
Published5 May
Down’s syndrome: Abortion case heads to High Court
Campaigners are set to have a review of abortion law relating to Down’s syndrome heard at the High Court.
Heidi Carter, of Coventry, and Máire Lea-Wilson from Brentford, west London, are challenging the government over a clause in the current law which allows abortion for up to birth for a foetus with Down’s syndrome.
Mrs Carter, 25, who has the condition, said the current law is “not fair”.
The case is due to be heard on 6 and 7 July.
Currently, there is a 24-week time limit for abortion, unless “there is a substantial risk that if the child were born it would suffer from such physical or mental abnormalities as to be seriously handicapped” .
Mrs Carter, who campaigns under her given name of Crowter, previously wrote to Health Secretary Matt Hancock saying all non-fatal disabilities should be subject to the same standard 24-week limit.
James and Heidi on their wedding day
image captionMrs Carter married her husband James last year
“A baby without Down’s syndrome can be aborted up to 24 weeks, but a baby like me and James can be aborted to birth,” Mrs Carter said. “It’s downright discrimination.”
“People shouldn’t be treated differently because of their disabilities.
“The reason it’s important to me and James is because we’re someone who has Down’s syndrome and we want to show the world we have a good quality of life.”
Mrs Lea-Wilson, 32, said she was placed under pressure to have an abortion when a 34-week scan revealed her son had Down’s syndrome.
Down’s syndrome ‘not something to fear’
‘We were offered 15 terminations of our baby girl’
Latest news from the West Midlands
“I have two sons that I love and value equally, but the law does not value them equally,” she said.
“My motivation for taking this joint legal action with Heidi has always been simple. As a mother, I will do all that I can to ensure the fair and equitable treatment of my son, Aidan.”
Mrs Lea-Wilson said the case is “not about the rights or wrongs of abortion” but about “removing a specific instance of inequality of the law.”
blob:https://www.channel4.com/1b543a29-8892-49b0-a2b6-8a0a04bec406
An officious woman’s voice, very early in the morning. She sounded panicked, “You have a 1 in 64 chance of having a Down’s baby, you will have to decide what to do”. This was my brush with Downs. I started to cry, not because of Downs but because her panic brushed on to me.
It was a miracle I was pregnant at all only having one fallopian tube and I was 42, an ‘elderly prim’ in those days. I was going to have a baby and a baby I was going to have…
I had private medical insurance in those days from the company I worked for and so for the second time I went to a Private Hospital on the South-Coast which was run by Nuns and which had an operating theatre in the basement. Each night, all night, for a week, a nun sat in the corner of my room watching over me. This had happened before when I had a parotid gland removed from my face, a very lengthy and skilful operation where miraculously I did not end up with a facial droop or other facial nerve problems. I was in my twenties for both major operations.
https://www.eastbourneherald.co.uk/heritage-and-retro/heritage/forty-nine-new-flats-could-be-built-former-eastbourne-private-hospital-2946657
https://www.eastbourneherald.co.uk/news/people/esperance-hospital-eastbourne-history-facility-prepares-closure-69929
The Doctor who took me off Seroxat cold-turkey went to extreme lengths in her denial, even suggesting that an ‘ectopic’ pregnancy’ was the cause of my Seroxat induced chronic distress. Considering my fallopian tube was removed with great skill and I was soon to move to the USA for my job, it seems just a little desperate to refer such private details to a psychiatrist, something she had not discussed with me and something which had occurred light years before my pregnancy.
Some other suggestions she had were equally arcane and toe-curling.
The Down’s issue stayed with me to a small degree, but after ‘that’ phone call no more was said from anybody.
The point is that whatever arrived, and this was a once-in-a-lifetime event, would be cherished and loved. There was no question about that and if my baby was anything like the joyful and inspiring Teresa Pocock then indeed I would have been blessed
Butterflies in My Stomach: Synopsis
This is the true story of Teresa Pocock, a woman with Down syndrome who has overcome discrimination and her own fears, to blossom into an award-winning artist and author. Four years ago, at age 49, Teresa was written off as “incapable” and was forced into a old-age nursing home in Ontario. Teresa did not want to live there. Her father and a sister rescued her, and Teresa moved across the country to B.C. to start a new life. “Butterflies in My Stomach” will tell her remarkable journey: How 26,000 people on Change.org, as well as civil rights organizations, and the media, helped Teresa get an apology from the government. And how Teresa’s new community in Vancouver, helped her to have confidence and emerge as a professional artist and a self-advocate.
https://www.billiamjames.com/butterflies-in-my-stomach/
overcoming discrimination —
Politics of Care – the NHS in UK is used as a political football locally and nationally – not always for the good of populations but of the party playing power games with voters. Some interesting points in this:-
Political appointees in the NHS—be careful what you wish for
The 2021-22 Health and Care Bill gives politicians new powers to control the detail of how the healthcare service runs. But past evidence suggests this may be unwise, unnecessary, and potentially damaging,
Following the publication of the 2021-22 Health and Care Bill [2], Nuffield Trust Chief Executive Nigel Edwards said:
“There is a clear logic to the parts of this Bill that would allow the NHS to collaborate more, as it has been trying to do for years in the face of the unhelpful 2012 Health and Social Care Act. But unfortunately these changes are bundled up with new powers for politicians to control the detail of how the health service runs. The evidence of the past suggests this may lead to worse decisions, and they will come to regret it.
From what i’ve seen in different places the more not just management but hierachies in orgs/groups of people the less well things work out either for those in receipt of ‘caring’
or employed in caring. even those in unpaid roles, whose expertise is trivialised. One ever lasting discontent is the imbalance of power beteen those who do the caring because they do care and those in ‘higher’ positions, particularly psychologists who have only done a few placements during an academic profession but ‘think they know best.’ In some ways they have expertise which ‘carers’ value but the reverse is not as valued. The happiest places I have known about have been where a division of status is not visible jargon is not used ‘team meetings’ are not called that and include everyone if at all possible (I think if this is not possible an advocate should be included) and somehow the most genuine of relationships develop based on something like mutual respect, ,even love. When there’s too much intereference in relationships being able to develop between all involved it becomes a more bureaucratic ‘service’ done to another person
For me it is “easy” to see the scale-problems with the complexity-lens.
There is dimensionalities (‘axis’) that if you scale you must change the dimension of procedure (if mechanical) or praxis (if human or “organic”). 1-on-1 clinical visit is a political event (by Levinas). 3 or more is when democracy starts (you need to “vote”). If you cook for your loved one, you will do things differently if you do a dinner for 15 people. Here technology can help you (even AFTER eating, like cleaning the mess. Here it doesn’t matter that the objects used are washed impersonally with washing machine and so on insted of with your hands and soup). But caring for your grandma is a different praxis compared to caring for a “stranger old woman” in your job and is different compared to caring for a 30 “strangers old men and woman” and is different compared to caring for a 220 from 09:00 to 13:00 in the morning with 4 minutes to every one of them.
The irony is that we are paying a lot for what “Pretty Woman” portrayed so good in the film (those who divided enterprise and sell them apart with more benefits that maintaining together the “package”) and we are paying very little those who really care for us (the speculators LITERALLY don’t care for us as long as we can’t be profitable for them. They have 0 compromise and only “answers” the market, that is LITERALLY no-one).
I am proposing a taxonomy of “Intimate Labors”:
https://www.amazon.com/Intimate-Labors-Cultures-Technologies-Politics/dp/0804761930
And blocking by law the “scale of care” to the smallest possible one. Better 10 nurse houses with 50 old people there than 1 with 500 old people there.
People are not hamburguers. And care is not scale-independent or scale-free. So, how we make this happen?
Could be the NH|S has gone too far down the drain already but maybe it’s still worth fighting for:- Keep Our NHS Public
Fund the NHS, not the private sector
1,280
Signatures
Target 2000
Please sign our petition to demand the UK Government invests £10 billion in the NHS – NOT in private healthcare.
First name
Last name
Email
I would like to join Keep Our NHS Public’s mailing list for more information about its campaigns and activities.
Sign
Opt In or Opt Out bearing in mond both Ben G and Matt H were intrumental in drawing it up and attempting to slip it in without informing the public or medics -There is no duty of care regarding any obligation by practitioners to inform those registered with them that they need to make this decision.There has been a stink in UK following the attempt at a population wide birth to death massive Data grab by politicians without consultation or information given to citizens so that the option to opt out of ‘sharing’ their data may be taken. Ben Goldacre was the lead for drawing up the proposal which has now been forced to hold back
‘The draft strategy also commits the DHSC to, where appropriate, act on the findings and recommendations of the Goldacre Review [1] into the use of data for research and analysis which is expected to conclude later on this year.’
The final version of the strategy is expected to be published later in 2021. In the meantime, the government has launched a consultation of stakeholders.
WHAT DOES THE DRAFT POLICY COVER?
The new strategy proposes central improvements to the way the data collected by the NHS (and other care providers) in England is used. The paper is split into 7 chapters each tackling a separate way in which patient data may be used to benefit the health and social care system and ensure a high quality of care.
The publication of the draft strategy policy comes in the wake of a general backlash against the controversial General Practice Data for Planning and Research (GPDPR) programme, purporting to transfer all GP records into a centralised database, a plan now expected to be postponed to 1 September 2021.T
Search
5 July 2021
UK NHSX NEW DATA STRATEGY FOR A POST-PANDEMIC WORLD: “TRANSFORMING HOW DATA IS USED AND SHARED IN HEALTH AND SOCIAL CARE: DATA SAVES LIVES”
IN THE LAST FIVE YEARS, MORE SCIENTIFIC DATA HAS BEEN GENERATED THAN IN THE ENTIRE HISTORY OF MANKIND
On 22 June 2021, the Department of Health and Social Care (DHSC) published its draft policy paper titled ‘Data Saves Lives,
The Cost of ‘Care’ – Pharma’s made a killing as the phrase goes. We’ll never know how many of the 6million prescriptions have led to harms and deaths as they are not recorded.
(This has been during the period when Matt Hancock was Health Minister in UK – many of his arrangements are being investigated.
In the Guardian last year
More than 6 million people in England received antidepressants in the three months to September, part of a wider trend and the highest figure on record.
And
Cost of sertraline has increased by more than 500% since …https://pharmaceutical-journal.com › article › news › co…Cost of sertraline has increased by more than 500% since 2019, figures show
Despite the number of items of sertraline dispensed increasing by 12% in 2020/2021, the cost increased by £142m, NHS data show.
Prescribing
14 June 2021By Julia Robinson
Sertraline blister pack
The NHS Business Services Authority said this was the second consecutive year that the cost of items dispensed in England had increased
The cost of the antidepressant, sertraline, to the NHS in England increased by more than 500% between 2019 and 2020/2021, despite the number of items dispensed only rising by 12% in that time, figures released by the NHS Business Services Authority (NHSBSA) have shown.
The annual Prescription Cost Analysis (PCA), published on 10 June 2021, includes information about the costs and volumes of prescriptions that have been dispensed in England over the past year.
Drugs containing the active ingredient, sertraline hydrochloride, increased in cost from £1.56 per item in 2019 to £8.89 per item in 2020/2021; an increase of 470%. As a result, the total cost to the NHS was almost £168m in 2020/2021, compared with just over £26m in 2019, an increase of 538%. This was despite the number of items prescribed increasing by just 12%, from 16.8 million to 18.9 million.
Sertraline (100mg tablets) was the presentation with the largest absolute increase in cost between 2019/2020 and 2020/2021, with an increase of £78.9m, from £21.0m to £99.9m, the PCA showed.
The 2020/2021 PCA also detailed that the cost of prescription items dispensed in the community in England had risen to £9.61bn — a 3.49% increase of £324m from £9.28bn in 2019/2020.
The NHSBSA said this was the second consecutive year that the cost of items dispensed in England had increased, following three consecutive years of decreases between 2015/2016 and 2018/2019.
The Pharmaceutical Journal reported in April 2020 that manufacturers had reported “industry-wide” supply challenges, exacerbated by export bans and border closures implemented as a result of the COVID-19 pandemic.
Overall, a study published in March 2021 found that the total number of antidepressant prescriptions dispensed in 2020 increased by 4 million compared to 2019 — costing the NHS England an extra £139m.
Steve Bazire, honorary professor at the School of Pharmacy at the University of East Anglia, said there had been “erratic” shortages of sertraline since the beginning of 2020, with the 100mg tablets in particularly short supply.
“My last trust has been able to source sertraline but from different suppliers each time and at varying costs; they currently pay around £5 for 28x100mg, but that does change from week to week according to who has what available,” he said.
Bazire said it appeared that the huge price increases were only being experienced in the UK.
A price concession — which is set when pharmacists may face difficulties in getting medicines at their usual prices owing to supply or other issues — was granted for sertraline 100mg and 50mg by the Department of Health and Social Care for the period April 2020 to October 2020.
This article was corrected on 15 June 2021 to clarify that the calendar year of 2019 is being compared with the financial year of 2020/2021 for some data.
My modest proposal: let’s take ninety-five percent of the money we spend on drugging senior citizens in nursing homes and use it to hire more nursing assistants and pay them more.